What is Bell’s Palsy?
Bell’s Palsy is a neurological condition that strikes unexpectedly, causing sudden weakness or paralysis of the facial muscles, typically on one side of the face. This mysterious disorder can be alarming, but understanding its nature is the first step toward effective management. Often mistaken for a stroke, Bell’s Palsy is actually a temporary condition caused by inflammation or compression of the facial nerve, which controls the muscles responsible for facial expressions.
Instagram reel
Symptoms and Diagnosis
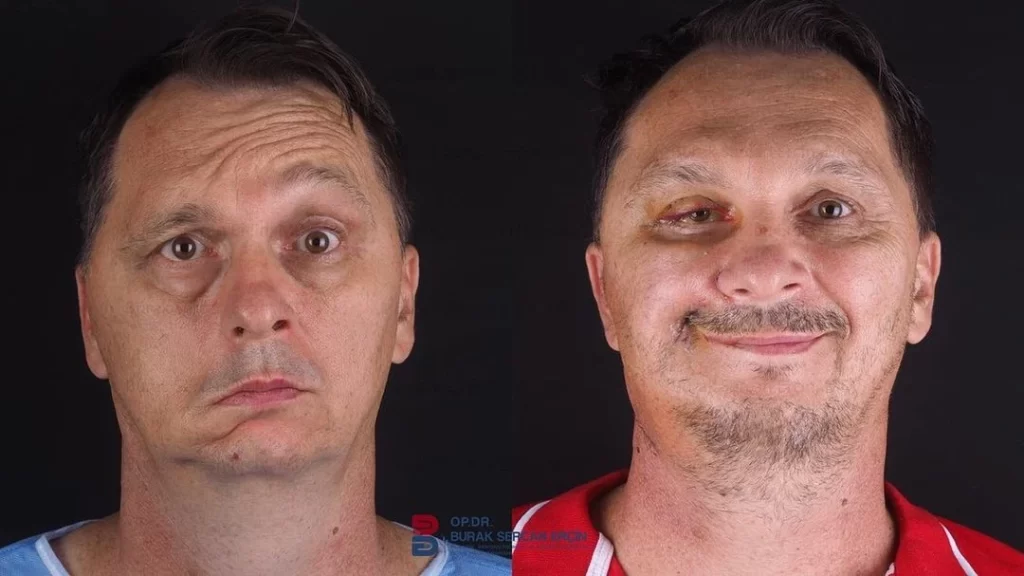
Recognizing Bell’s Palsy early can make a significant difference in treatment outcomes. Key symptoms include:
- Sudden drooping on one side of the face
- Difficulty closing one eye
- Inability to make facial expressions
- Drooling or difficulty eating
- Sensitivity to sound
- Headaches or pain behind the ear
Diagnosis typically involves a comprehensive medical examination. Healthcare professionals will rule out other potential causes like stroke or brain tumor through physical assessments and potentially imaging tests like MRI or CT scans.
Treatment Options for Bell’s Palsy
Bell’s Palsy Surgery
While surgery is not the primary treatment for most Bell’s Palsy cases, it can be considered in rare, complex situations. Surgical interventions might be recommended when:
- There’s significant nerve damage
- Symptoms persist beyond six months
- Physical therapy and medications show limited improvement
Facial nerve decompression surgery and nerve grafting are advanced techniques that can help restore facial nerve function in challenging cases.
Medications
Corticosteroids
Corticosteroids are the frontline medical intervention for Bell’s Palsy. Medications like prednisone work by reducing nerve inflammation, potentially accelerating recovery and preventing long-term complications. Typically prescribed within 72 hours of symptom onset, these powerful anti-inflammatory drugs can significantly improve outcomes.
Antiviral Drugs
Some physicians may prescribe antiviral medications, particularly if a viral infection like herpes is suspected as the underlying cause. While their effectiveness is still being studied, they might provide additional support in the healing process.
Physical Therapy
Benefits of Facial Exercises
Physical therapy is a game-changer in Bell’s Palsy recovery. Specialized facial exercises can:
- Prevent muscle atrophy
- Retrain facial muscles
- Improve nerve communication
- Reduce the risk of permanent facial asymmetry
Patients work with therapists to develop personalized exercise routines that gently stimulate and rehabilitate affected facial muscles.
Alternative Therapies
Acupuncture
This ancient healing technique has shown promising results for some Bell’s Palsy patients. By stimulating specific nerve points, acupuncture may:
- Reduce inflammation
- Improve nerve function
- Alleviate pain
- Support overall healing process
Massage Therapy
Gentle massage techniques can complement traditional treatments by:
- Improving blood circulation
- Reducing muscle tension
- Promoting nerve healing
- Supporting lymphatic drainage
Coping with Bell’s Palsy
Emotional and Psychological Support
Bell’s Palsy can be more than just a physical challenge—it’s an emotional journey that tests one’s resilience and self-confidence. The sudden change in facial appearance and functionality can trigger a range of intense emotions, from frustration and anxiety to depression. Recognizing and addressing these psychological impacts is crucial for holistic recovery.
Support strategies include:
- Joining support groups (both online and in-person)
- Seeking counseling or therapy
- Practicing stress-reduction techniques like meditation and mindfulness
- Connecting with others who have experienced Bell’s Palsy
- Maintaining open communication with family and friends
Remember, your emotional healing is just as important as your physical recovery. It’s okay to feel vulnerable, and seeking help is a sign of strength, not weakness.
Lifestyle Adjustments
Navigating daily life with Bell’s Palsy requires practical adaptations and self-care:
- Eye care: Use artificial tears and an eye patch to protect the affected eye
- Eating modifications: Use a straw, cut food into smaller pieces
- Skincare: Protect the affected side of the face from wind and extreme temperatures
- Communication: Be patient with yourself and others
- Nutrition: Consume foods rich in B vitamins and anti-inflammatory nutrients
- Rest and stress management: Prioritize sleep and relaxation
These adjustments can help manage symptoms and support your body’s natural healing process.
Assoc. Prof. Dr. Burak Sercan Consultation in Turkey
For patients seeking specialized care, Assoc. Prof. Dr. Burak Sercan is a renowned expert in neurological disorders, particularly Bell’s Palsy, based in Turkey. With extensive experience in diagnosis, treatment, and rehabilitation, Dr. Sercan offers comprehensive care that combines cutting-edge medical techniques with a compassionate approach.
Key highlights of Dr. Sercan’s approach:
- Personalized treatment plans
- Advanced diagnostic techniques
- Multidisciplinary treatment strategy
- Focus on both medical and psychological recovery
- International patient support services
Patients from around the world seek Dr. Sercan’s expertise for his holistic and innovative approach to Bell’s Palsy management.
How does Bell’s Palsy impact a person’s physical and emotional health?
Bell’s Palsy significantly impacts both physical and emotional health, often striking unexpectedly and causing a range of functional and psychological challenges.
Physical Health Impacts
The primary physical impact of Bell’s Palsy is the sudden weakness or paralysis of the facial muscles, typically occurring on only one side of the face. This occurs due to the inflammation or compression of the facial nerve. Specific physical consequences include:
• Functional Impairments: Individuals often experience sudden drooping of the face, making it difficult to close one eye or create normal facial expressions. This can lead to practical difficulties such as drooling or trouble eating, often requiring modifications like using a straw or cutting food into smaller pieces.
• Sensory and Neurological Issues: The condition can cause sensitivity to sound, headaches, or sharp pain behind the ear.
• Secondary Complications: Without proper intervention, there is a risk of muscle atrophy and permanent facial asymmetry. Additionally, because the affected eye may not close properly, patients must take active steps to protect it using artificial tears and eye patches to prevent damage.
• Physical Tension: The condition can lead to increased muscle tension in the face, which is often addressed through massage therapy to improve circulation and promote healing.
Emotional Health Impacts
The emotional toll of Bell’s Palsy is often as significant as the physical symptoms, as the sudden change in one’s appearance can be deeply distressing.
• Psychological Distress: The abrupt loss of facial control and the resulting change in appearance can trigger intense emotions, including frustration, anxiety, and depression.
• Impact on Self-Confidence: Because the face is central to communication and identity, the condition frequently tests a person’s resilience and self-confidence. Patients often report feeling a sense of vulnerability as they navigate social interactions with altered facial functionality.
• Stress of Daily Adaptation: The need for constant lifestyle adjustments—such as managing eye care and navigating communication difficulties—adds a layer of daily stress that requires patience and mental fortitude.
Recognizing that emotional healing is just as vital as physical recovery is a cornerstone of effective management. Support strategies, such as counseling, support groups, and mindfulness, are recommended to help patients cope with the psychological weight of the disorder. While the journey can be daunting, most cases resolve within a few months, and maintaining a positive mindset is considered a key factor in accelerating the healing process.
Is Bell’s Palsy Permanent?
One of the most common concerns patients have after a Bell’s Palsy diagnosis is whether the condition will last forever. The reassuring answer for most people is no — Bell’s Palsy is typically not permanent. However, understanding the factors that influence recovery can help patients set realistic expectations and take the right steps early.
How Often Bell’s Palsy Becomes Permanent
The majority of Bell’s Palsy patients — roughly 70–85% — experience significant or full recovery within three to six months. In cases where treatment begins promptly (ideally within 72 hours of onset), recovery rates are even higher. A smaller percentage of patients may experience lingering weakness or asymmetry, particularly if the nerve damage was severe or treatment was delayed.
Signs Recovery Is Happening
Knowing what to watch for can offer real peace of mind. Positive signs that your facial nerve is healing include:
- Gradual return of movement in the forehead or around the eye
- Reduced stiffness or tightness in the affected side
- Improved ability to close the eye fully
- Returning sensation and taste
- Symmetry slowly evening out during expressions
When Nerve Damage Becomes Long-Term
In a minority of cases, particularly those involving complete nerve disruption rather than compression or inflammation, some degree of permanent facial weakness can occur. Risk factors for prolonged recovery include late treatment initiation, age over 60, high blood pressure, and diabetes. Incomplete recovery after 12 months is generally considered a sign of lasting change.
Treatments That Improve Recovery Chances
Early and consistent intervention dramatically reduces the risk of permanent damage. The most effective approaches include:
- Corticosteroids started within 72 hours of symptom onset
- Facial physiotherapy to prevent muscle atrophy
- Eye protection to avoid corneal damage from incomplete eye closure
- Surgical options such as facial nerve decompression in severe, non-responding cases
If you are concerned about your recovery trajectory, consulting a specialist in facial nerve conditions is the most important step you can take.
Bell’s Palsy Recovery Timeline
Recovery from Bell’s Palsy is rarely a straight line : it unfolds in stages, and understanding what to expect at each phase can reduce anxiety and help patients engage more effectively with their treatment.
First Week: Acute Phase
The first week is typically the most intense. Symptoms often reach their peak within 48–72 hours of onset. During this period:
- Facial weakness or paralysis is most pronounced
- Eye closure may be difficult or impossible
- Speech and eating can feel awkward
- Pain behind the ear is common
This is the critical window for starting corticosteroids and, if recommended, antiviral medication.
Weeks 2–3: Early Improvement Phase
For many patients, subtle signs of improvement begin to appear. Patients often notice:
- Slight return of movement at the corner of the mouth or eyebrow
- Reduction in pain behind the ear
- Less pronounced drooping during rest
Physical therapy should be well underway at this stage, reinforcing nerve pathways through targeted facial exercises.
Months 1–3: Active Recovery Window
This is the period when the most visible progress typically occurs. The facial nerve, which regenerates slowly at approximately 1mm per day, begins to re-establish communication with the muscles. During this phase:
- Facial symmetry gradually improves
- Muscle strength returns progressively
- Some patients notice full recovery by week 8–10
Consistency with physiotherapy is especially important here to guide correct muscle retraining and prevent synkinesis (abnormal muscle co-contractions).
Months 3–6: Final Recovery & Assessment
By the six-month mark, most patients have reached their recovery plateau. Those with mild-to-moderate Bell’s Palsy will typically have fully recovered. For cases involving more severe nerve involvement, residual weakness may persist and surgical evaluation may be considered at this stage.
Signs the Facial Nerve Is Healing
- Return of voluntary facial movement
- Improved eye closure (able to fully shut the eye)
- Symmetrical smile and forehead wrinkling
- Restored sensation and taste on the affected side
Patience is key. The facial nerve is one of the slowest-healing nerves in the body, and some patients continue to improve beyond the six-month mark.
What Happens in Mild Bell’s Palsy Cases?
Not all Bell’s Palsy cases are the same. A significant number of patients present with mild weakness rather than complete facial paralysis — and their outlook is generally excellent. Understanding how mild cases differ from severe ones helps patients avoid unnecessary alarm and focus on the right recovery steps.
Symptoms of Mild Bell’s Palsy
In mild cases, patients typically experience partial weakness on one side of the face rather than full paralysis. Common presentations include:
- Slight drooping at the corner of the mouth
- Mild difficulty fully closing the eye
- Reduced expression on the affected side
- Subtle asymmetry most noticeable when smiling or raising the eyebrows
- Minor speech changes or difficulty with certain sounds
Importantly, most patients with mild Bell’s Palsy can still partially close their eye, eat without significant difficulty, and maintain most facial movements.
Recovery Speed in Mild Cases
The good news for mild cases is that recovery is typically faster and more complete. Many patients with mild Bell’s Palsy see meaningful improvement within two to four weeks, with full recovery often achieved by weeks six to eight. Studies consistently show that patients with incomplete paralysis at onset have the best prognosis.
Treatment Differences
Even in mild cases, treatment is still recommended. Key approaches include:
- Corticosteroids: Often still prescribed to reduce nerve inflammation and support faster recovery, even when weakness is partial
- Eye care: Lubricating eye drops are still advised if eye closure is even slightly incomplete
- Facial exercises: Light physiotherapy helps maintain muscle tone and speed up nerve recovery
When to See a Doctor
Even if symptoms feel minor, prompt medical evaluation is important. Bell’s Palsy must be correctly diagnosed to rule out other causes of facial weakness such as stroke, Lyme disease, or a parotid gland tumor. A doctor will also assess the degree of nerve involvement using clinical grading scales, which guides treatment decisions.
If your symptoms are mild and improving within the first week, that is an encouraging sign. However, any facial weakness that does not begin improving within three weeks warrants specialist review.
Eye Problems in Bell’s Palsy and How to Treat Them
Because the facial nerve controls the muscles responsible for closing the eyelid, Bell’s Palsy often causes incomplete or complete inability to shut the eye on the affected side. This creates a serious risk of corneal damage if not properly managed — and eye care should be considered a priority from the very first day of diagnosis.
Why Bell’s Palsy Affects the Eye
The facial nerve (cranial nerve VII) controls the orbicularis oculi muscle, which is responsible for closing the eyelid. When this nerve is inflamed or compressed, the eyelid may not fully close — a condition called lagophthalmos. As a result, the cornea is left exposed to air, dust, and dryness, increasing the risk of corneal ulceration or infection.
Artificial Tears and Eye Lubrication
The first line of protection for the Bell’s Palsy-affected eye is consistent lubrication. Recommendations typically include:
- Daytime: Preservative-free artificial tear drops used frequently throughout the day (every 1–2 hours in severe cases)
- Nighttime: A thicker lubricating eye gel or ointment applied before sleep to prevent overnight dryness
- Monitoring: Regular self-checks for redness, pain, blurred vision, or light sensitivity, which may indicate corneal involvement
Eye Patching
For patients whose eye does not close fully, an eye patch worn during sleep — or throughout the day in severe cases — provides a physical barrier against dryness and environmental irritants. Moisture chamber glasses (sealed eyewear that retains humidity) are another option for daytime use, particularly in dry or windy environments.
Taping the Eyelid Shut
Some specialists recommend gently taping the eyelid closed at night using medical-grade tape. This is a simple and effective way to prevent overnight corneal exposure while the nerve recovers. Patients are instructed on proper technique to avoid irritating the eyelid skin.
Eyelid Surgery for Bell’s Palsy
In cases where significant lagophthalmos persists beyond several months and conservative measures are no longer sufficient, surgical options may be considered. These include:
- Gold or platinum weight implantation: A small weight is placed in the upper eyelid to assist gravity in closing the eye. This is reversible and often recommended as a temporary or permanent measure depending on recovery progress.
- Tarsorrhaphy: A partial stitching together of the upper and lower eyelids to reduce the exposed eye surface. This can be performed temporarily or permanently.
- Lower eyelid tightening procedures: To address ectropion (outward turning of the lower lid) caused by muscle weakness.
Eye-related surgical interventions are generally considered when nerve recovery has stalled and corneal health is at ongoing risk. An ophthalmologist should be involved in the care of any Bell’s Palsy patient with significant eye closure difficulties.
Can Bell’s Palsy Be Cured?
The question of whether Bell’s Palsy can be cured is one that patients ask almost immediately after diagnosis — and the answer depends on how we define “cure.”
Most Cases Resolve Fully
For the majority of patients, Bell’s Palsy resolves completely over time. The facial nerve regains its full function, and no visible signs of the condition remain. In this sense, Bell’s Palsy is indeed “curable” — not through a single treatment, but through the natural healing process supported by timely medical intervention.
Studies suggest that approximately 70–85% of patients with Bell’s Palsy achieve full recovery, and this figure rises further when treatment with corticosteroids is started within the first 72 hours.
Treatment Accelerates Recovery — It Doesn’t Override It
No medication or therapy directly “cures” Bell’s Palsy in the way an antibiotic cures a bacterial infection. Instead, treatments work by creating the best possible conditions for nerve healing:
- Corticosteroids reduce inflammation around the facial nerve, giving it space to recover
- Physical therapy prevents muscle atrophy and guides proper nerve-to-muscle reconnection
- Eye care and lifestyle adjustments prevent secondary complications that could complicate healing
The goal of treatment is to shorten recovery time and minimize the risk of permanent weakness — not to cure the nerve damage directly.
Cure vs. Recovery: Understanding the Difference
It is important to distinguish between cure and recovery. A cure implies the underlying disease mechanism is eliminated. Bell’s Palsy involves a triggered inflammatory or viral event that damages the facial nerve — once the nerve heals, the condition resolves. Recovery, in this context, is the process of the nerve regaining its function.
For patients who experience incomplete recovery, ongoing management — including physiotherapy, botulinum toxin injections for synkinesis, or surgical reconstruction — can significantly improve quality of life even when full cure is not achieved.
When Should You Expect Resolution?
- Mild cases: Often resolve within 4–6 weeks
- Moderate cases: Most recover within 3–4 months
- Severe cases: Recovery may take up to 12 months, with some residual weakness in a small percentage
If you have been diagnosed with Bell’s Palsy, the most important action you can take is to begin treatment early and follow up with a specialist if improvement is not apparent within three weeks.
Conclusion
Bell’s Palsy, while challenging, is not an insurmountable condition. With the right combination of medical treatment, physical therapy, emotional support, and lifestyle adjustments, most patients experience significant improvement and can regain their facial function.
The journey may seem daunting, but remember:
- Most cases resolve within a few months
- Early intervention is key
- A positive mindset accelerates healing
- You are not alone in this experience
Always consult healthcare professionals, stay informed, and approach your recovery with patience and hope. Your resilience is your greatest asset in overcoming Bell’s Palsy.