This article was written by Assoc. Prof. Dr. Burak Sercan Erçin and is based on clinical experience. A specialist in Plastic, Reconstructive and Aesthetic Surgery; prepared in accordance with current medical literature and personal surgical data. A consultation is recommended before making any medical decisions.
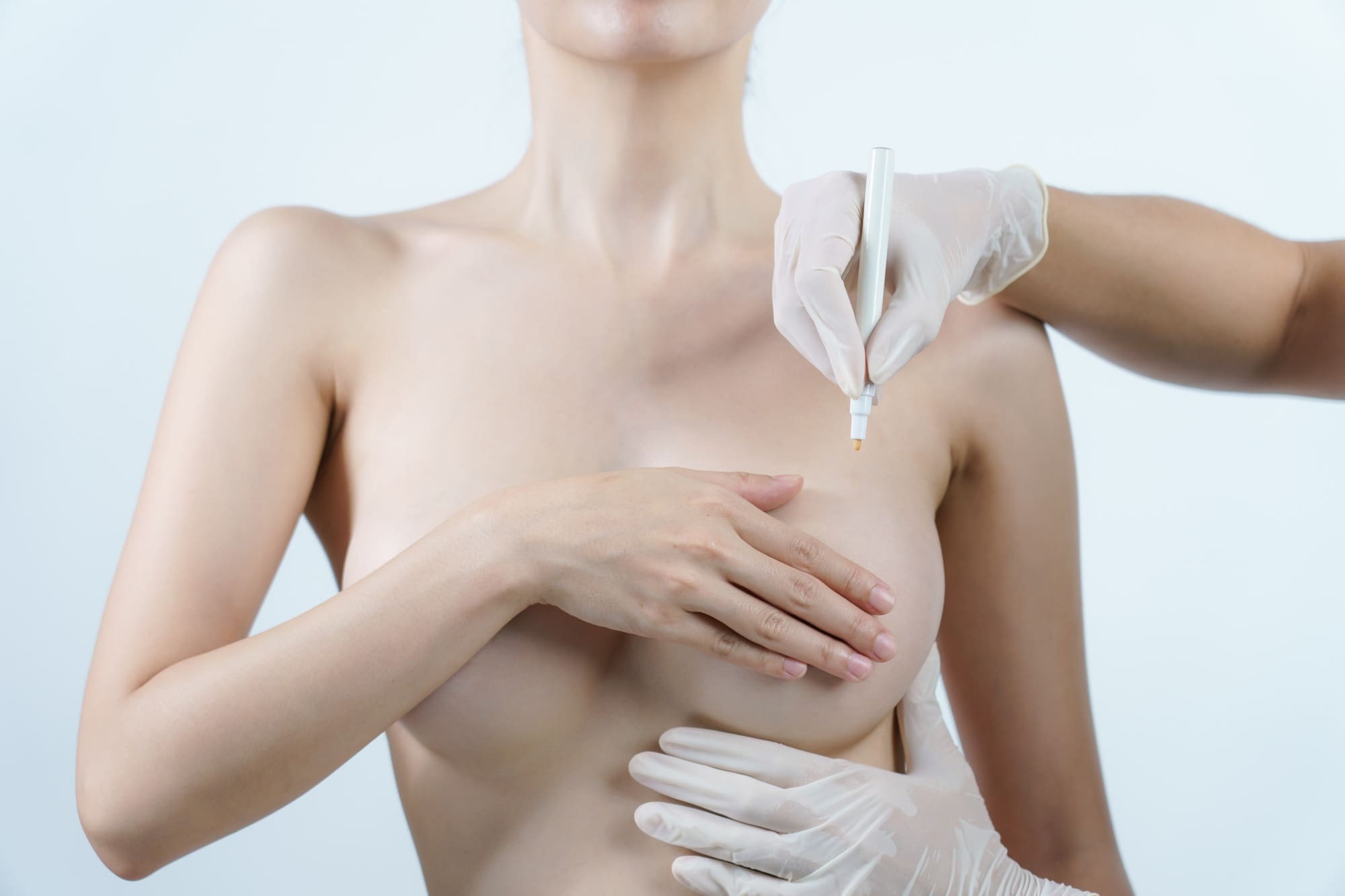
Especially women who have had a mastectomy or lumpectomy and then undergo breast reconstruction surgery often report that it changed their lives. As a sign of power and resilience in the face of breast cancer, this treatment can aid in restoring a sense of womanhood, confidence, and wholeness.
What Is Breast Reconstruction Surgery?
After a mastectomy or lumpectomy, a patient’s self-esteem and quality of life might benefit greatly from breast reconstruction surgery. Every patient’s needs can be met with a tailored approach thanks to the wide variety of procedures available such as breast augmentation, including both TRAM Flap and DIEP Flap.
In most cases, it all starts with a talk with a plastic surgeon who focuses on breast reconstruction and has passed the appropriate board exams. The surgeon will look through the patient’s medical records, talk about the patient’s desired outcomes, and advise them on the best course of action during this introductory consultation.
When a patient chooses TRAM Flap, either silicone or saline implants are placed in the chest area to simulate a healthy breast. Nevertheless, in DIEP Flap reconstruction, the patient’s own tissue is used to reconstruct the breast. This tissue can come from the patient’s tummy, back, or buttocks. As the tissue transplant is matched to the patient’s own body, the outcomes are often more natural.
How Should I Prepare Before Breast Reconstruction?
There are numerous ways to prepare for breast reconstruction after cancer and get the best results. Breast reconstruction preparation tips:
- Consult with a plastic surgeon: The first step in breast reconstruction preparation is to visit a board-certified plastic surgeon. The surgeon will examine your medical history, discuss your goals of care, and assist you in choosing the best option during this initial meeting.
- Medical history: Your surgeon should know about all your operations, medical conditions, and medications. This will assist the surgeon to choose the most secure and efficient method.
- Stop smoking: Smokers should cease at least three weeks before reconstruction after mastectomy. To avoid issues, stop smoking.
- Eat healthy: A diet rich in fruits, vegetables, lean protein, and whole grains will help your body prepare for surgery and heal afterward.
- Reduce stress: Stress can weaken your immune system and make it difficult to heal after surgery. Relaxation techniques can prepare you for the surgery and ensure a good recovery.
- Plan for post-surgical help: After breast reconstruction after mastectomy, you’ll need help with domestic chores and transportation. For a few days or weeks after the treatment, you may need help with cooking, cleaning, and bathing.
Follow these steps to achieve the greatest breast reconstruction after mastectomy result and easy recovery.
How Painful Is Breast Reconstruction Surgery?
An extensive operation, and breast reconstruction after cancer require incisions to be made and tissue to be manipulated in the chest. Breast reconstruction, like any operation such as breast augmentation surgery, causes pain, but the severity varies.
Most people have chest pain and discomfort after the surgery. When the body heals, pain medication reduces this discomfort. The surgery type affects pain.
When the implants settle and the wounds heal, those who have undergone a TRAM flap may feel tightness, edema, and discomfort in the chest area. Over-the-counter or surgeon-prescribed painkillers can relieve the pain.
DIEP flap may cause additional breast pain and suffering, especially in the tissue-harvesting area (such as the abdomen or back). This procedure requires lengthier incisions and tissue treatment, thus healing is longer.
Is Breast Reconstruction a Major Surgery?
Breast reconstruction after mastectomy or lumpectomy often necessitates general anesthesia and cutting-edge surgical methods. Different patients have different needs, thus the surgeon doing the breast reconstruction after cancer can choose from a variety of techniques.
TRAM Flap restoration uses silicone or saline implants to restore breasts. DIEP Flap surgery uses the patient’s own tissue from the abdomen, back, or buttocks to restore the breast.
Breast reconstruction after a mastectomy is complicated and requires a qualified plastic surgeon. Patients may anticipate taking time off work and avoid hard activity for a few weeks after the surgical treatment. With sufficient care and assistance, most patients can return to their daily tasks within several weeks or months and have a successful surgery.
How Long Does Breast Reconstruction Surgery Take?
Several types of surgery and individual factors can affect how long it takes to complete the surgical procedure. This treatment might take one to 8 hours.
It is common for TRAM Flap to be a faster surgical process than DIEP surgery. The surgery involves chest incisions, pocket creation, and implant placement. The surgery takes two to three hours.
Nevertheless, DIEP reconstruction procedures usually take more time than implant-based procedures. Depending on tissue harvesting and rebuilding difficulty, this procedure can take several hours.
This surgery may be done in stages, with the first surgery establishing the groundwork for the rest. Before ultimate reconstruction, the patient’s breast tissue may need to be stretched or extended.
Depending on your unique situation and the method of reconstruction being used, your plastic surgeon will be able to give you a more precise time estimate for your treatment.
What Are the Risks of Breast Reconstruction Surgery?
The surgery carries with it a range of risks and potential consequences that can be specific to the procedure, the patient, and their medical history.
The surgery may cause:
- Hematomas can arise from heavy bleeding during or after surgery.
- Each surgical operation carries the danger of infection in the wound area or around the implant.
- The surgery can cause breast pain, especially in the initial few days and weeks.
- The surgery might leave scars, especially around incisions.
- Implant rupture, displacement, and capsular contracture can occur with breast implants (a tightening of the tissue capsule around the implant).
- Tissue flap reconstruction risks include insufficient blood supply, tissue loss, and flap failure.
- The surgery can alter breast and nipple sensations.
If you’re considering this surgery, talk to your cosmetic surgeon about the benefits and drawbacks of the procedure.
What Should Be Considered After Breast Reconstruction Surgery?
To recuperate smoothly and get the greatest results from breast surgery, follow these instructions. Consider:
- Post-op recommendations: Your surgeon will explain how to care for the incision site, relieve pain, and look after yourself during recovery. Follow these recommendations to reduce complications and increase healing.
- Attend follow-up consultations: You may need to see your plastic surgeon in the months and days after surgery. Your surgeon checks for problems and progress throughout these appointments.
- Start taking care of your incision site: Good care reduces infection risk and promotes healing. Keep the wound dry and clean and maintain your surgeon’s dressing or bandage guidelines.
- Handle pain and discomfort: Breast surgery often causes breast pain and discomfort. To alleviate this pain, your surgeon may recommend or suggest over-the-counter painkillers.
- Let time heal: Breast surgery is a serious process, so relax and recover. After surgery, rest and don’t lift heavy objects for several weeks.
- Seek support: The surgery is both physically and emotionally draining. Talk to a professional, support group, or your family and friends for help.
These methods and collaborating with your plastic surgeon will help you recover after mastectomy reconstruction and get the finest results.
What is the Softest Boob Job?
The “softest” boob job often refers to the result that feels most like natural breast tissue—both to the patient and to the touch. The softness depends on factors such as implant type, placement, surgical technique, and the patient’s own anatomy. Silicone gel implants, especially the newer generation of “gummy bear” cohesive gel implants, tend to feel softer and more natural than saline-filled alternatives. Additionally, subglandular placement (above the muscle) can allow for a more natural feel, although submuscular placement (beneath the muscle) may be recommended for long-term results and reduced risk of complications.
Surgeons may also combine fat grafting with implants to achieve ultra-soft, natural-feeling results. This technique uses a patient’s own fat (harvested from the abdomen, thighs, or flanks) to add volume and smooth edges around the implant. The result is a hybrid breast augmentation that blends the benefits of structure and softness.
Can You Feel Breast Implants Inside Your Body?
While breast implants are designed to mimic the feel of natural breast tissue, whether or not you can “feel” them inside your body depends on several variables. Patients with thinner skin, low body fat, or subglandular placement may notice the implant edges more easily, particularly in the upper chest or sides. In contrast, patients with more tissue coverage or implants placed beneath the chest muscle usually experience a more integrated feel.
Modern implant technologies have significantly improved comfort. Over time, most patients adapt to the presence of implants and describe them as a seamless part of their body. However, it’s important to note that changes in sensation, mild tightness, or awareness of the implant can occur, particularly in the early months post-surgery. Open communication with your surgeon during consultation can help manage expectations regarding how natural the implants will feel for your specific body type.
New Breast Reconstruction Techniques
Breast reconstruction techniques have advanced considerably in recent years, offering patients more natural-looking, durable, and personalized outcomes. One of the most notable innovations is prepectoral implant placement, where implants are positioned above the chest muscle, minimizing animation deformity and often reducing pain and recovery time.
Autologous reconstruction has also evolved, with procedures like DIEP flap (deep inferior epigastric perforator) gaining popularity. This technique uses a patient’s abdominal tissue—without sacrificing muscle—to reconstruct the breast, resulting in a natural look and feel with fewer donor-site complications.
Fat grafting, either on its own or in combination with other methods, has become a widely accepted way to fine-tune shape and softness. Some clinics also offer 3D-printed tissue scaffolding, a promising frontier in regenerative reconstruction that supports tissue regeneration in more complex cases.
Finally, nipple-sparing mastectomies and immediate reconstruction procedures allow for fewer surgeries and more aesthetically pleasing outcomes. These techniques are often personalized based on a patient’s anatomy, cancer treatment history, and aesthetic goals—emphasizing a tailored, patient-first approach in modern breast reconstruction.
How Breast Reconstruction Can Help You Love Your Body Again
Restoring a woman’s self-esteem and feeling of femininity following breast cancer treatment or other traumatic events can be accomplished through a significant surgical procedure known as breast reconstruction. It’s possible to reconstruct the breasts in a number of ways, including with implants or a tissue flap. Proper planning, post-operative care, and follow-up sessions can minimize risks and promote recovery after surgery.
At the Burak Sercan Ercin Clinic, we specialize in both reconstructive surgeries such as Facial Paralysis, Hand Surgery etc. and aesthetic surgeries such as breast reconstruction surgery, Rhinoplasty, Liposuction, Tummy Tuck, Breast Aesthetics and more that will restore a woman’s confidence in her physical appearance. Make an appointment with one of our skilled and caring plastic surgeons today if you’re thinking about this surgery.
Breast Reconstruction Surgery Before and After
Breast reconstruction surgery can be a transformative journey—physically and emotionally. Before surgery, patients often experience a wide range of emotions including anxiety, hope, and uncertainty, especially if reconstruction follows a mastectomy. The preoperative phase includes imaging, surgical planning, and sometimes tissue expansion, depending on the chosen method (implant-based or autologous reconstruction).
Post-surgery, the body begins to heal and adapt. The “after” phase typically reveals not only a restored breast contour but also a renewed sense of body image and confidence. It’s important to remember that final results evolve over time. Swelling may persist for weeks or months, and revisions or nipple reconstruction may be part of the longer process. Many patients report improved self-esteem, greater wardrobe freedom, and a feeling of closure as they see their silhouette restored.
Before-and-after photos are powerful tools that illustrate the possibilities of breast reconstruction. These visuals also help set realistic expectations by showing variations based on body type, surgical technique, and healing patterns.
This content was written by Assoc. Prof. Dr. Burak Sercan Erçin in line with clinical experience and current medical literature. It is intended for general informational purposes only and does not constitute medical advice. A personal consultation with Dr. Erçin is recommended for individual assessment.

Faculty Member · Bahçeşehir University
Graduate of Ege University Faculty of Medicine, Assoc. Prof. Dr. Erçin completed advanced fellowships at Tampa General Hospital (USA) under Dr. Deniz Dayıcıoğlu in breast reconstruction and burn surgery, and at the clinic of Dr. Pedro Cavadas in Valencia, Spain in reconstructive microsurgery. After passing the EBOPRAS examination in 2018, he joined Bahçeşehir University as a faculty member and continues his private practice on Bağdat Avenue, Istanbul, specialising in face, breast and body aesthetics alongside complex reconstructive surgery.