This article was written by Assoc. Prof. Dr. Burak Sercan Erçin and is based on clinical experience. A specialist in Plastic, Reconstructive and Aesthetic Surgery; prepared in accordance with current medical literature and personal surgical data. A consultation is recommended before making any medical decisions.
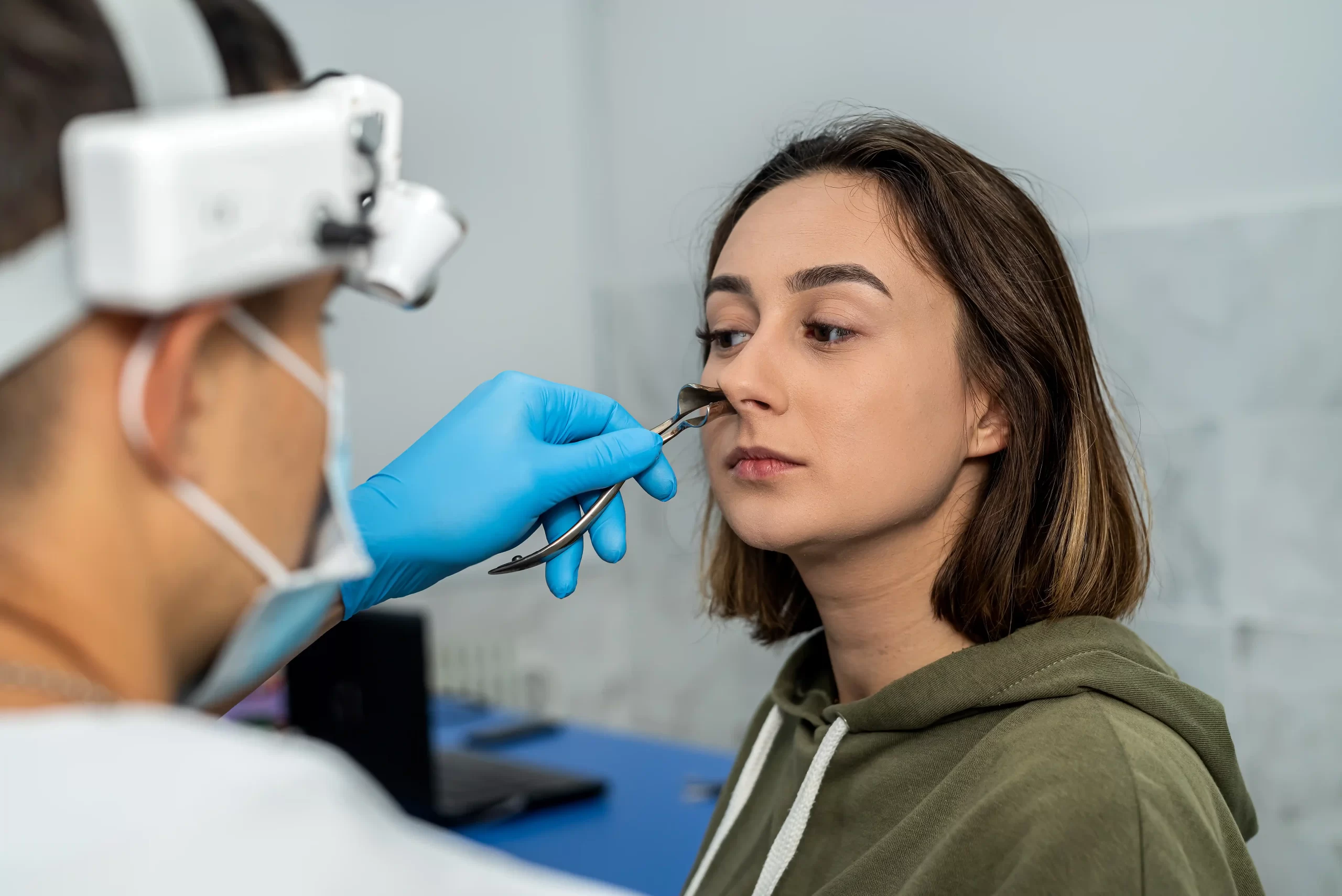
Nasal reconstruction is a surgical procedure aimed at rebuilding the nose’s form and function. Rhinoplasty (a “nose job”) can be either cosmetic or reconstructive. Reconstructive rhinoplasty restores structure after trauma, congenital deformity or disease, whereas cosmetic rhinoplasty only changes appearance.
For example, severe nasal fractures (a broken nose) often require reconstruction to realign the bones and cartilage and restore breathing. Similarly, individuals who have had a previous unsatisfactory rhinoplasty, congenital deformities (like a cleft nose), or nasal tissue loss from tumors or burns may also need nasal reconstruction. In each case, a skilled surgeon can reconstruct the nose to restore both its natural appearance and normal airway function.
Types of Nose Reconstruction Procedures
Nose reconstruction can involve different techniques, depending on the cause of deformity:
- Traumatic (“Broken Nose”) Repair: Injury to the nose from sports or accidents can fracture the nasal bones and tear cartilage. Ideally a fresh fracture is reset within days; if the nose heals crookedly, a delayed reconstructive rhinoplasty is planned after 6–12 weeks. Trauma often produces a crooked (“S”- or “C”-shaped) nose, a collapsed (“saddle”) bridge, or septal perforations. Reconstructive rhinoplasty realigns the bones and cartilage, often adding grafts (e.g. from septum, ear or rib) to rebuild the nasal framework and restore normal shape and breathing.
- Revision Rhinoplasty: If a previous nose job left you unhappy (cosmetically or functionally), a revision procedure may be needed. These cases are more complex because of scar tissue. Experts note that scar tissue can make rhinoplasty up to ten times more difficult. I specialize in revisions: I carefully free any scarred areas and add cartilage or structural grafts to achieve the desired look and airway improvement.
- Congenital/Developmental Deformities: Some patients are born with nose deformities that need correction. For example, a cleft lip/palate often causes a flattened tip and deviated septum. Repairing these anomalies involves rebuilding the cartilage framework and reshaping tissues for symmetry. Correcting congenital issues can greatly improve both appearance and nasal airflow. Other developmental asymmetries (like uneven nostrils from birth) are handled similarly.
- Oncologic and Burn Reconstruction: When nasal tissue is lost to skin cancer removal or burns, reconstruction often uses tissue flaps and grafts. A common solution is the paramedian forehead flap, where skin from the forehead (with its blood supply) is rotated down to cover a large nasal defect. Smaller wounds may use cheek flaps (nasolabial flaps) or skin grafts. Cartilage grafts are placed underneath to rebuild support. In these complex cases, I reconstruct the nose so it both looks natural and functions normally, even after major tissue loss.
- Ethnic Rhinoplasty: Patients of different ethnicities (Middle Eastern, Asian, African, etc.) often seek rhinoplasty that respects their heritage. Techniques are chosen to refine the nose while preserving ethnic features. As one study cautions, applying a standard “Western” nose model to other ethnic groups can lead to breathing problems and revision surgeries. Instead, I tailor each approach: for example, subtly narrowing a broad bridge or refining a wide tip so the result looks harmonious with the patient’s face and culture.
In all these scenarios, I evaluate each case individually. The ultimate aim is the same: to restore a healthy, natural-looking nose that breathes easily.
Key Differences Between Aesthetic and Functional Reconstruction
It’s important to distinguish aesthetic rhinoplasty from functional reconstruction, though most surgeries involve both. Aesthetic rhinoplasty focuses on appearance: changing the nose’s shape, size or proportions (for example, reducing a hump or refining a tip). Functional rhinoplasty focuses on airway function: straightening a deviated septum, opening clogged passages, or reinforcing weak support to improve breathing.
In practice, comprehensive nose surgery addresses both goals together. For example, a deviated septum (septal reconstruction) not only obstructs breathing but often makes the nose look crooked. Correcting the septum thus fixes both issues. Conversely, cosmetic changes (like narrowing a wide nose) often require placing grafts to maintain internal support. I always examine both aspects: when reshaping for appearance, I ensure the airway remains open; when fixing function, I pay attention to the external look. One review describes rhinoplasty as a procedure that “restores the form and function of the nose”, which is exactly the outcome I aim for.
Ethnicity adds another layer to this balance. For instance, surgeons note that using a one-size-fits-all (Caucasian) approach on Asian, African or Middle-Eastern noses can create problems. Therefore, I adapt techniques to each patient’s features. The result is a nose that looks aesthetically pleasing and is functionally normal – truly integrating form and function.
How to Prepare for Surgery
Proper preparation leads to a smoother recovery. Here’s what to expect:
- Consultation and Planning: We start with a detailed consultation. I review your medical history, examine your nose inside and out, and may order imaging (CT scans, 3D photographs) to understand the structure. Often I use 3D imaging or simulation software (such as Lindapp) to show you expected changes. We discuss your goals openly; I will explain what changes are realistic given your anatomy. You can ask as many questions as you like. By the end of this visit, we will have a clear plan for surgery.
- Medical Preparation: You may need routine pre-op tests (blood work, EKG if age-appropriate, etc.). Stop smoking at least 4–6 weeks before surgery to promote healing. Discontinue blood-thinners or anti-inflammatories (like aspirin, ibuprofen, vitamin E) about a week prior, after checking with any other doctors you see. Arrange for someone to drive you home after surgery and stay with you at least the first night or two.
- Logistical Planning: If you’re traveling from abroad, we can conduct a preliminary video consultation. Once surgery is scheduled, you can arrange travel. Plan for about 7–10 days off work or school for initial recovery. We will provide written instructions on fasting (nothing by mouth after midnight before surgery) and other pre-op details.
- Setting Expectations: Rhinoplasty recovery is gradual. I will explain that while you may see visible improvement quickly, the final result takes time. A small amount of swelling, especially in the tip, can persist for many months. We will discuss potential risks and the likely timeline so you know exactly what to expect.
In summary, preparing well means being medically ready (healthy, on schedule for tests and medications) and mentally prepared (understanding the process). My team and I will guide you through each step so you feel confident and informed before your surgery.
Surgical Techniques Used (Grafts, Cartilage, Open vs Closed)
Nose reconstruction employs a variety of advanced techniques:
- Closed vs Open Rhinoplasty: In a closed rhinoplasty, all incisions are inside the nostrils (no visible external scars). This is suitable for minor reshaping. In an open rhinoplasty, a small incision is made on the columella (the tissue between the nostrils). This allows me to lift the skin and see the nasal cartilage and bone directly. I typically use an open approach for major reconstructions (fractures, graft placement, complex revisions) because it provides maximum visibility and precision, at the cost of a tiny (hardly noticeable) scar.
- Cartilage Grafts: Cartilage is the framework of the nose. Whenever possible, I use your own septal cartilage (from inside your nose) for grafts. This cartilage can be reshaped and placed as spreader grafts, tip grafts or struts to support the new structure. If the septum doesn’t have enough cartilage, I may harvest cartilage from your ear (conchal cartilage) or your rib (costal cartilage). For example, rib cartilage provides plenty of strong material for rebuilding a collapsed bridge or columella in severe cases. All grafts are carved precisely and secured with sutures. The body then incorporates this cartilage as new nasal support.
- Tissue Flaps and Grafts: For skin or lining defects, tissue flaps are used. A classic example is the forehead flap, where forehead skin (with its blood supply) is rotated to the nose to cover large wounds. This skin matches the nose in color and texture, making it ideal for major reconstructions. For smaller defects, I can use a cheek flap (nasolabial flap) or even a bilobed flap. In some cases, a full-thickness skin graft is placed on the outside or inside of the nose. Any donor scars (forehead, cheek, ear, rib) are closed carefully to minimize visibility.
- Osteotomies and Suturing: Often, the nasal bones must be gently fractured and reset (osteotomies) to narrow a wide nose or straighten a crooked one. Inside the nose, I use fine suturing techniques to reshape cartilage and secure grafts. I often use dissolvable sutures for internal work so that no stitches need removing later. The skin is redraped smoothly over the new framework.
In all procedures, I apply splints or gentle taping on the outside for support and to maintain the new shape. Throughout the surgery, I focus on preserving or restoring your nasal airway. The combination of these techniques – open access, cartilage grafts, flaps, and precise suturing – allows me to reconstruct even severely damaged noses into ones that look natural and breathe normally.
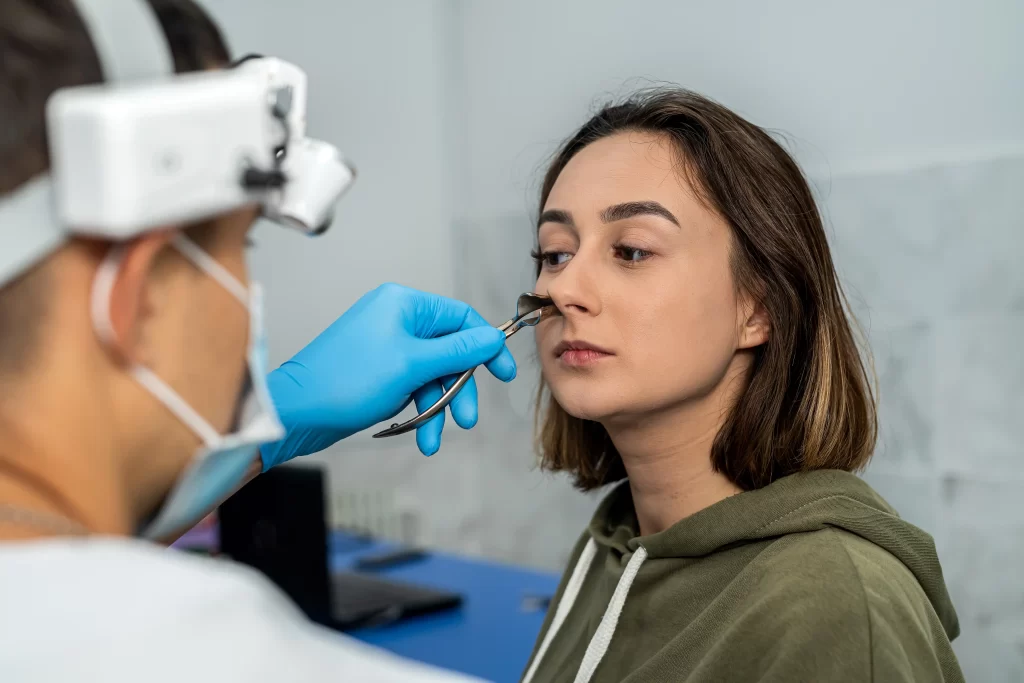
During rhinoplasty, cartilage structures are exposed so the surgeon can graft or reshape them. In this image, the lower lateral cartilage is visible inside the nose.
Recovery Process: Week by Week
Recovery after nose reconstruction is gradual. Here is a typical timeline:
- Week 1 (Days 0–7): Your nose will be supported with an external splint and possibly internal packs or stents. Expect significant swelling and bruising around the eyes and nose. Pain is usually mild and managed with medication. Keep your head elevated and apply cold compresses for the first 2–3 days. The splint and any visible stitches are left in place for about 7 days. Rest and avoid strenuous activity – your priority is healing.
- Weeks 2–3: Around day 7–8, the splint and dressings are removed. Bruising should be mostly gone by the end of the second week. By now the nose will look noticeably better, though it still feels a bit swollen. Many patients feel well enough to return to work or school during week 2. (As one report notes, most people resume normal activities about 1–2 weeks after surgery) Continue to avoid heavy exercise or anything that might risk bumping your nose. You should breathe much more easily now that the septum is straightened, although mild congestion may persist.
- Month 1: At four weeks, a large portion of the swelling has subsided and the nasal bones have healed fully. The nose’s shape should look much like it will ultimately. You may still notice some slight fullness (especially at the tip) that only you can see or feel. I will see you for a 1-month check; we often discuss scar care or gentle massage at this point. Most patients can resume most normal activities now (except contact sports).
- Months 2–3: Healing continues internally. By 2–3 months, nearly all remaining swelling is gone. Your nose should look and feel natural. Any numbness inside the nose is gradually subsiding. We usually have a follow-up visit around 3 months to ensure everything is on track. At this point you should be very satisfied with the appearance and breathing improvement.
- Months 4–12: The final subtle refinements happen slowly. The nasal tip, in particular, may continue to settle and refine for up to a year. By 6–12 months, your nose has essentially reached its final shape. I typically schedule a final review at 12 months to confirm that healing is complete.
Throughout recovery, I monitor your progress closely. My team provides instructions on nasal hygiene (saline rinses, ointments) and activity. We encourage gentle care and avoiding any trauma. Remember: while the majority of healing occurs in the first few weeks, the final result takes months to fully mature. Patience is key, but rest assured that each week you will look and feel better. Our goal is that you end up with a nose that looks natural and allows you to breathe fully.
Risks, Complications, and How They’re Minimized
All surgeries carry risks, and I will discuss them with you in advance. For nasal reconstruction, potential issues include:
- Bleeding or Hematoma: Some bleeding and nasal drainage is normal initially. Rarely, a significant blood clot can form inside the nose; this would require prompt drainage to prevent pressure damage. To reduce this risk, I control bleeding meticulously during surgery and may place gentle pressure packs if needed.
- Infection: Nose surgery has a low infection rate, but it’s possible. I use sterile technique and often prescribe antibiotics as a precaution. If any sign of infection (redness, fever, pain) occurs, I treat it immediately.
- Scarring or Wound Healing Issues: Incisions inside the nose leave no visible scar, but external incisions (columella, donor sites like the forehead) can heal with fine lines. I close all skin incisions carefully to minimize scars. Smoking or medical conditions can impair healing, which is why I insist on smoking cessation and managing conditions like diabetes beforehand.
- Breathing Problems: Paradoxically, surgery can make airflow worse if not done carefully (e.g. if too much cartilage is removed). I avoid this by preserving and reinforcing the nasal valve and septum. In some cases I may widen the internal valves (spreader grafts) to improve breathing. After surgery, I check that both sides of your nose are open.
- Cartilage Graft Issues: In rare cases, a cartilage graft can warp slightly or shrink. To prevent this, I carve grafts with precision and sometimes oversize them so they settle to the intended shape.
- Unfavorable Cosmetic Result: Despite all efforts, some irregularity or asymmetry may remain. I discuss realistic expectations and show before/after examples. If needed, a minor revision can be considered after full healing.
Despite these possibilities, most patients experience tremendous benefits: improved breathing, restored symmetry, and boosted confidence. In reviews of reconstructive surgeries, common complications like infection or bleeding are well-known but infrequent. My experience (15+ years) means I can anticipate and prevent most problems. Throughout your care, we follow strict protocols to minimize risks. For example, I handle tissues gently, use fine sutures, and monitor you closely post-op.
If any complication does occur, we act quickly. A hematoma would be drained immediately, infections treated promptly, and so on. My follow-up schedule is designed so we see you often in the first weeks, catching and managing issues early. In my practice, major complications are very rare, and the vast majority of patients heal without trouble and achieve excellent results.
Why Choose Me (Credentials, Approach, Testimonials)
I am Dr. Burak Sercan Erçin – an Associate Professor of Plastic and Reconstructive Surgery with over 15 years of experience. I completed my medical degree and plastic surgery residency in Turkey, then pursued advanced fellowships in the USA (breast reconstruction) and Spain (microsurgery). I am board-certified and hold international credentials (such as EBOPRAS). I am also active in research and education, with publications on reconstructive techniques.
In my practice, I combine scientific knowledge with an artistic eye. I take that to heart in every surgery. I listen carefully to my patients’ goals and explain the plan clearly. I often use 3D imaging to show expected outcomes, which helps set realistic expectations. During surgery, I am methodical and precise – using magnification if needed and fine instruments – to achieve the best possible result.
My patients consistently praise the care they receive. They say I communicate well and involve them in decisions. For example, one patient wrote, “From the initial consultation to follow-up, everything was explained so well. Dr. Erçin and his team made me feel comfortable, and the result was amazing – I breathe so much better now.” Another stated, “I came for a revision rhinoplasty, and Dr. Erçin understood exactly what I wanted. He fixed my nose beautifully and showed great compassion.” These testimonials, along with high ratings on international review, reflect my commitment to patient satisfaction.
In short, you can trust my expertise: years of reconstructive experience, academic background, and a track record of happy patients. Under my care, your nose will be rebuilt with the utmost skill and care.

International Patients: Travel, Language, Aftercare Coordination
I welcome patients from the USA, UK and around the world. Istanbul is well-connected (direct flights from major cities) and offers modern medical facilities. Here’s what international patients can expect:
- Language and Communication: I speak fluent English, as does my entire team. You will have no trouble discussing your case. We can start with a video consultation from home to go over your needs. All consent forms and instructions will be in English.
- Logistics: We can provide a letter of medical consultation or treatment to help with any visa process. Upon arrival, an airport pickup can be arranged if needed. I operate at VM Medical Park Pendik Hospital (Istanbul), a modern, internationally accredited hospital. Private rooms and English-speaking nurses are available. My staff can assist you in finding nearby accommodations if needed.
- Medical Care: Your care will follow the same high standards as for local patients. You will have pre-op workups (labs, imaging) and meet the anesthesiologist before surgery. After surgery, you’ll stay in a comfortable room. We schedule all necessary follow-up visits during your stay here.
- Aftercare: Once you return home, I continue to follow your progress. I will provide detailed discharge instructions in English. We schedule follow-ups by phone or email, and I am available for any questions. If you have a doctor back home (ENT or plastic surgeon), I can coordinate care with them if needed. You will be asked to send pictures or have a video check-in so I can see how you are healing.
- Experience: Many international patients report a smooth journey. Our patient coordinators guide you through every step, from hotel booking to answering questions about Turkey. You focus on your recovery, and we handle the rest. With us, you get world-class nose reconstruction and support every step of the way.
Rest assured, traveling for surgery has become routine for many of our patients. We aim to make it easy and transparent so you can have peace of mind.
Conclusion: Regain Form and Function with Expert Care
Nose reconstruction can profoundly improve your quality of life – restoring the ability to breathe freely and boosting confidence in your appearance. With my extensive reconstructive expertise, especially for international patients, you can achieve a safe and satisfying outcome.
This guide has explained what nasal reconstruction entails: the various procedures (trauma repair, congenital correction, revision rhinoplasty, etc.), the difference between cosmetic and functional goals, how to prepare, the surgical methods I use (grafts, flaps, open vs closed), the recovery timeline, and the risks. Above all, my priority is that your nose will look natural and function normally.
If you or someone you know needs nose reconstruction surgery, remember that skilled care makes all the difference. Under my care, you will indeed regain both the form and function of your nose. I look forward to helping you achieve a nose that you can be proud of.
This content was written by Assoc. Prof. Dr. Burak Sercan Erçin in line with clinical experience and current medical literature. It is intended for general informational purposes only and does not constitute medical advice. A personal consultation with Dr. Erçin is recommended for individual assessment.

Faculty Member · Bahçeşehir University
Graduate of Ege University Faculty of Medicine, Assoc. Prof. Dr. Erçin completed advanced fellowships at Tampa General Hospital (USA) under Dr. Deniz Dayıcıoğlu in breast reconstruction and burn surgery, and at the clinic of Dr. Pedro Cavadas in Valencia, Spain in reconstructive microsurgery. After passing the EBOPRAS examination in 2018, he joined Bahçeşehir University as a faculty member and continues his private practice on Bağdat Avenue, Istanbul, specialising in face, breast and body aesthetics alongside complex reconstructive surgery.